
Бесплатный фрагмент - COPD
COPD
Book Blurb
“COPD: Chronicles of Survival” — is a raw and honest diary of a man who has been fighting for every breath for over 20 years. The author journeys from an active life to being tethered to an oxygen concentrator, sharing unique insights: from the technical nuances of medical equipment to personal trials of cutting-edge peptide therapies. This is a book about maintaining spirit when oxygen levels hit 77%, and how the love and devotion of family become the ultimate medicine.

Preface
We abuse nature with our emissions, and nature retaliates with a disease — COPD.
Back in my student days, one could pass an exam in Strength of Materials and then, just a day or two later, pass Philosophy. But when you are writing books, it is difficult to switch from philosophy to “strength of materials.” In my previous books, I shared stories that happened to me throughout my long life and wrote about those who were by my side. Much that remains unwritten in the form of stories will die with me.
I truly do not want to be nothing more than a meaningless photograph on a gravestone for my grandchildren. People do not die when their hearts stop beating; they die when the memory of them fades — that is when they truly turn into just an old photograph. But just as manuscripts do not burn, memory preserved in books does not die.
In none of my previously published books did I mention that I have been living with COPD (Chronic Obstructive Pulmonary Disease) for twenty-five years. Average readers aren’t interested in that; they want a gripping plot, not the author’s struggles. Moreover, twenty-five years of fighting for your life is not the kind of anniversary that relatives and friends come to congratulate you on. What kind of “anniversary” can COPD even have? It carries only a life sentence.
I thought about this for a long time and finally concluded that I was wrong! There is a target audience that is not looking for a twisted plot, but specifically for a description of my challenges — especially considering that COPD is the third leading cause of death worldwide, trailing only heart attacks and ischemic diseases. Furthermore, in the wake of COVID—19, the number of people with lung issues has surged. Such books often become bestsellers.
These readers do not need the digitized perspective of a doctor looking at a CT scan; they need the perspective of a fellow patient, expressed in friendly language. That is why I decided to write. I only regret that I did not keep an observation diary; imagine how much useful information could have been gathered over 25 years!
COPD is not a term for a single specific illness, but an umbrella term used to describe chronic lung diseases that lead to airflow limitation. It is not just a simple “smoker’s cough,” but an underdiagnosed, life-threatening lung condition.
Dear readers, COPD — especially in its late stages — is very serious and, above all, agonizing. If a criminal is sentenced to hanging, they are hanged, and that is the end of it. A COPD patient, however, is sometimes “hanged” daily. Usually, the ambulance manages to take the patient out of the “noose,” but only so that they might end up in it again the very next day!
I am not a doctor treating COPD. I am something else — I am a COPD patient with, terrifyingly enough, 25 years of experience. I am alive thanks to a naturally strong constitution and — I am not afraid of this word — the heroism of my wife.
Risk Factors
The primary risk factors for COPD include:
— Smoking
— Occupational hazards (working in harmful industries)
— Atmospheric pollutants (contact with harmful particles in the air, burning landfills, and smoke from large factories).
I fell ill during a time when Georgia was without electricity, gas, or water for 10 years, from 1993 to 2003. It was a terrible time. We slept fully clothed… and in 1998, I got sick. Naturally, considering I smoked like a chimney back then — smoking everything that produced smoke — it was one of the primary reasons for my COPD.
We must also mention heredity. I have read very little about this, and what I did find was often buried in convoluted medical jargon. However, I have something to say on the matter: both of my grandmothers suffered from asthma (since, just like sex, “there was no COPD in the USSR”). My uncle from Rostov also had lung problems, and my beloved niece (a Tbilisi artist) also suffers from bronchial asthma. And, of course, your humble servant suffered from bronchitis and pneumonia since childhood, usually enduring them on my feet… because my grandmother’s favorite phrase was “it will heal before the wedding.”
But… it didn’t heal.

Let’s Talk About COPD
I want to warn you in advance — my texts will likely not be peppered with medical terms. Of course, I could go online and write… “lung parenchyma” — the sponge-like tissue of the respiratory organ — but I think that after two or three such terms, my readers would scatter.
COPD — Chronic Obstructive Pulmonary Disease — is a life-threatening condition where the airways steadily narrow due to chronic inflammation of the bronchi or emphysema. This disease is not always diagnosed in time, which significantly increases its danger.
COPD is one of the most common chronic lung diseases worldwide, affecting more than 300 million people. It ranks 3rd among the leading causes of death globally, following heart attacks and strokes.
COPD comes in two types:
As you can see from the illustration above, these two types are not the same. I never heard a word about this from doctors. Therefore, I strongly advise you to determine exactly which type of COPD you have — even just by external signs — because different types require different medications.
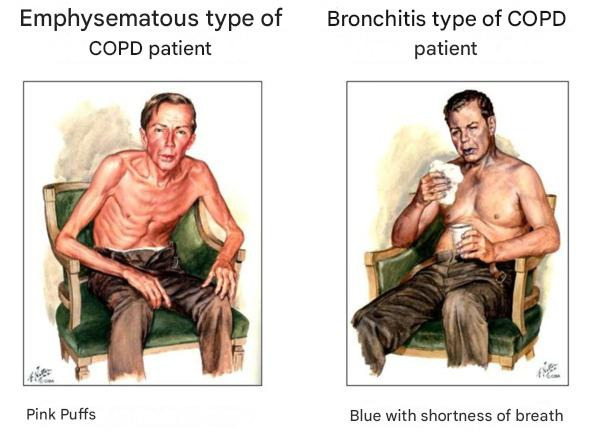
I cannot say anything specific about the first type, as I suffer from the second type. With this type, you won’t see your ribs; instead, you might gain 30—40 kg and develop a “beer belly”. Fight excess weight immediately — excess weight is the ENEMY!
— Emphysematous Type: Characterized by an expanded capillary network, low body weight, and shortness of breath. The intercostal spaces on the affected side are retracted and sharply narrowed. There is a pathological expansion of the internal lung cavities, where tissues are unnaturally stretched and inflated. A so-called “valve mechanism” occurs — air enters the tissues easily but exits with great difficulty.
— Bronchitic Type: Characterized by a wet, productive cough not caused by other diseases. Increased body weight and a bluish tint (cyanosis) of the skin indicate a lack of oxygen in the blood.
I gathered my experience bit by bit, mostly through trial and error. This stands in contrast to doctors, who are often focused on impressing the patient with their level of electronics, abundance of terminology, gestures, and smiles. They listen only cursorily to the symptoms the patient timidly tries to squeeze out, and are happy to insist how lucky you are to have come specifically to them — because as a “professional,” it is nothing for them to defeat the disease in a couple of weeks.
One of these “Aesculapians” once told me straight out: I won’t sew you moccasins, but as for curing you… it’s as easy as pie. But time went by, and the money earned through my back-breaking real estate work began to flow from the pockets of my red business jacket into the pockets of this doctor’s white coat. I think that with my money, he paved the road from his house to the hospital with two layers of asphalt. He would have been better off sewing moccasins.
And here is one more small piece of advice: if your city hospital receives a complex diagnostic machine along with, let’s say, a saxophone — do not think that learning to operate that machine is easier than blowing a melody on the saxophone. It’s just that when someone lies to you on a saxophone, you will realize it — but when a doctor lies to you about a diagnosis, you won’t.
Always keep that in mind!
Ten Years Without Light or Gas
Tbilisi survived for ten years without electricity, gas, or running water. Starting in 1993, gas supplies to Georgia were cut off, and restoration only began in the late 90s. The central heating system was completely destroyed. Consequently, boiler houses as such simply no longer exist in Georgia — today, everyone has their own individual heating system, depending on what they can afford.
In that situation, people found themselves at the center of a terrifying experiment: “Try to survive without gas, electricity, or heat”.
Electricity in Tbilisi was supplied on a rolling schedule. Power was turned on during peak hours in the morning from 8:00 to 10:00, and then again in the evening when people returned home — at best from 19:00 to 22:00. After that, a total blackout would begin again.
During the winter, local power grids constantly failed due to overload. As a result, entire districts would live without light — and consequently without water — for three or four days at a time. People stayed warm and cooked food using kerosene stoves. Those who could not afford kerosene warmed themselves with firewood.
It was a common sight to drive home and see a city in total darkness: no street lighting at all, with only car headlights visible. Public electric transport — trolleys, trams, and the metro — often stood idle. Over those ten years, trolleys and trams vanished from the city entirely: the rails were sold for scrap metal, and the contact wires for non-ferrous metal. Hospitals faced blackout schedules of 2—3 hours, while shops and offices adapted as best they could.
Georgia lived in this mode until 2003, when Mikhail Saakashvili’s team came to power.
A quarter of a century ago, Georgia was left without natural gas and electricity. People lit bonfires on city streets, lined up for firewood, and transportation did not run.
How many “smokers” with weakened lungs like mine fell ill with COPD during that reckless decade?
Non-Fiction
I have written and published five books of short stories and novellas. Everything was simple there: a section for humor, a section for stories, a section for miniatures. You just copy the text and paste it into the right part of the book. A book can be created in a day or two. But with non-fiction — especially when you are writing about health issues — there are problems.
If you are writing fiction, in one story you can be swimming in a pool, in another you can be a hostage, and in a third, a State Prize laureate. But now, imagine that I am a COPD patient: in one story, I write about how hard it is to breathe; in the second, about getting a kidney transplant; and in the third, about learning to walk on prosthetics. It doesn’t work that way — in every story, I have to write about how difficult it is to breathe, and one must be a virtuoso to avoid repeating oneself, especially since I never originally intended to write a book about myself and COPD.
Therefore, let’s agree right now: there will be no humor pieces, no miniatures, and certainly no novellas or novels in this book. There will be only one section — COPD, and the order of the articles and stories will be arbitrary.
I am being asked to write about this most unpleasant disease of our time, which has already climbed to third place in mortality rates — COPD. Well then, I will write, but not from a scientific point of view. I am not a medic, and even if I wrote like one, it would be of little use to an ordinary patient. It would be like reading Newton’s binomial theorem to milkmaids. I will write about what I felt at the beginning of the illness, what I did, and what should not have been done.
This is an experience that once cost me dearly — both financially and psychologically. I will write as clearly as possible so that those who must follow the path I have already traveled do not wander among doctors with a pleading, loyal gaze like a dog, hoping that the secret to recovery will be revealed to them.
Do not rely on a doctor’s Hippocratic Oath. Everyone takes an oath of some kind — some take a vow, some an oath of office, some a promise. The police swear to protect the people, judges swear to be honest, and we promise — not to cheat on our wives.
Ten years ago, when I was in Kiev as a foreigner, a fellow lung patient was in the next bed, and we ate together. A good guy, but after tests that lasted almost a week, he turned out to be tubercular!!! Thank God, I dodged that bullet, but I might not have…
In the early stages of the disease, when I couldn’t understand anything myself, I was mostly a “cash cow” for the doctors. During examinations, I was “passed around in circles” — they sent me everywhere except, perhaps, to the proctologist. Every doctor found something in me that, as they assured me, led to my breathing problems. Even with my straight Greek nose, they found a deviated septum that absolutely had to be corrected surgically, claiming it would solve all my problems. My wife saved the doctor’s nose that day.
So, in the initial period, be especially vigilant: the rescue of a drowning person is the work of the drowning person themselves. I am exaggerating a bit, but not much, considering the level of medicine in the countries of the former USSR.
In the following posts, using my own example, I will tell you how the disease developed. What circles of hell I went through just because I couldn’t find the right doctor. Those who tried to treat me didn’t even know exactly what to do or what to treat!
And now for the most important thing! It is hard to overestimate the fact that my wife, a fragile-looking woman, is constantly by my side. She has carried on her shoulders what is usually distributed among all family members; Lika carries everything alone.
It seems that it is love that turns women into “Joans of Arc”!
COPD and Its Progression
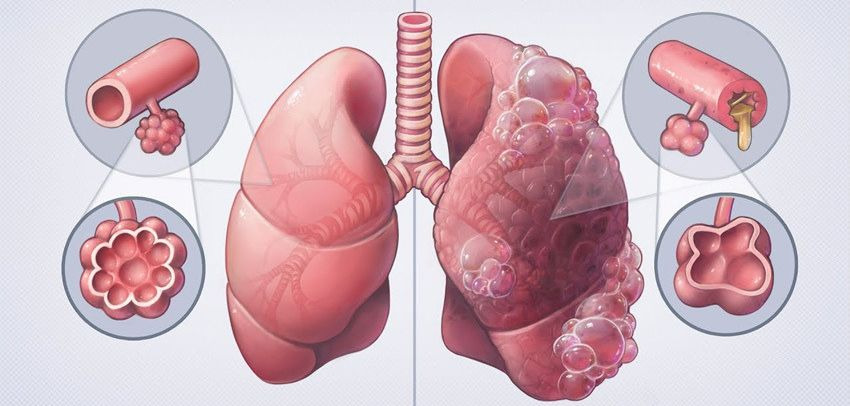
Unfortunately, COPD is incurable. The only thing one can achieve is a prolongation of the disease’s timeline and the creation of relatively comfortable living conditions. I will be writing
about the reality in the post-Soviet space, as conditions in the West are different — I haven’t lived there, so I won’t comment on them. In our region, people survive with this for 4—6 years, up to… well, the upper limit depends, unfortunately, on the availability of financial means, as prevention and maintenance are expensive.
I remember back in the USSR era, pharmacies would fill “oxygen pillows”. I filled one myself when my grandmother was dying of asthma. Today, it seems ridiculous — like licking a Validol tablet during a heart attack. Yet even today, somewhere in the middle of nowhere, they might still suggest an oxygen pillow for a choking fit — even in this age of oxygen concentrators and cylinders.
I can count the “mandatory” medications I consume on one hand. Some appear and disappear as needed — those that regulate blood pressure, heart function, flu medications, antibiotics, and so on. I won’t write about them specifically because every drug has multiple analogs depending on where it’s manufactured, and these drugs affect every individual differently at various stages of the illness. You must either determine what works through trial and error or consult with knowledgeable doctors.
I will tell you only about Salbutamol (known in the USA as Albuterol). Occasionally — though rarely — it can cause a paradoxical bronchospasm in the respiratory system. Ten years ago, Salbutamol was my “emergency aid” for stopping attacks. I held it in my hands constantly, just as today’s youth holds a smartphone. Even more so — when I used to swim in the pool (God, was there really such a time?), the inhaler was in my hand even then.
I don’t even need to mention that I had one canister at home, another in the car, a third in my pocket, and a fourth in my hand. I didn’t take a single step without it. But one day, due to its side effects, I ended up in the hospital, where they barely managed to save me. After that, I quit it cold turkey (as if I had quit smoking), though for about a year, I still couldn’t psychologically force myself to take it out of my pocket.
Now, it has been replaced by the oxygen concentrator. (Compare this to those oxygen pillows that only gave you 5—10 breaths).
That is why I wrote earlier that this is not a disease for pensioners — due to a lack of funds, they die sooner and more painfully than those who can afford maintenance therapy. I have read a lot about this condition and realized long ago that COPD is not the name of one specific illness, but a general term for various lung diseases accompanied by choking and oxygen deficiency. And what else should lungs lack besides oxygen, if their primary purpose is to saturate the blood with this gas?
I have met many “COPDers” in real life and online, and I noticed that the disease manifests differently in everyone:
— Some lose weight and look like a splinter.
— Others gain significant weight — for example, I gained about 30 kg.
— Many suffer from a wet cough with phlegm.
— I, on the other hand, do not cough at all unless I have a cold. But if I do cough, clearing my throat is extremely difficult and often leads to an attack.
I stopped seeing doctors a long time ago; somehow, I managed to stabilize my condition myself. Usually, when I was at a pulmonologist’s appointment, I would try to tell them about my observations and nuances, but I always heard the same thing:
“I know, I know, don’t strain yourself. We’ll have you back on your feet in a week, maybe two”.
And immediately, they would give me referrals for countless tests and examinations by specialists ranging from dentists to proctologists. It felt like they took me for an idiot. In reality, they were simply taking advantage of a patient’s desperation to get well, shamelessly trying to rob them.
However, I have also met “Doctors from God,” whom I don’t just applaud, but whom I owe my life to — thanks to them, I am writing this article today instead of lying in a graveyard. I will write more about one such doctor later — a true specialist who helped me fight the disease and a great person who eventually became a friend.
Comments on the COPD Article
These comments were written in response to an article I published in Livejournal in 2020.
Yuri T. Hi, Yur. COPD in your rendition is needed. Even if not as literature, it will at least help someone practically. Not everyone has the chance to stumble upon a good doctor — there aren’t many of them, as you know. Something truthful and, most importantly, personal is always useful for those suffering. And if it’s also literary — then it’s a real gift. Yur. (Egor41)
yurayakunin (Author) Yuri, thank you, my friend. You caught the theme perfectly. Of course, I don’t intend to write from a doctor’s perspective, but from a perspective that many doctors are unaware of (thank God) — that is my goal. I’ve been lucky to meet good people on my life’s journey, you being one of them, as well as good doctors. I feel somewhat indebted to those who were less fortunate. So, I want to share what I know.

Milana V. Please, write about COPD. My husband was diagnosed 8 months ago, so I really need to know what we will face and how I can support him. Thank you.
yurayakunin (Author) Milana, Milana, prepare for a long defense and a struggle for a comfortable living space. No illusions — people with amputated legs don’t hope they will grow back; they live with prosthetics, and the quality of life depends only on the quality of those prosthetics. I’m speaking metaphorically, of course; a person with good prosthetics can live a long and happy life, as much as someone who has adapted to them and to life with them can.
Unfortunately, for us, COPD patients, things are less rosy. We need a lot from those who surround us. To be honest — we are DYING at about the same rate as people with multiple sclerosis, in terms of speed. In the USSR, patients with COPD, bronchial asthma, chronic bronchitis, or emphysema died 1—3 years after diagnosis. Today, things are better; I’ve lived for 20 years and think I’ll last at least another year.
First — quit smoking immediately (one month of smoking equals minus one year of life!).
It would be great to gather a “COPD thread” based on one of my posts, where patients could share their experiences on how they keep their spirits up, or even help those who cannot fight due to lack of resources. If I hadn’t been gifted an oxygen concentrator TWICE!!! (the first was used, left after someone’s husband passed, and the second — a new one — when the first broke), I would have objectively died 6—7 years ago.
And most importantly, don’t rush to the doctors in luxury clinics. Many have a “Ferrari” but can only ride a “bicycle.” Don’t pay for their ownership of a Ferrari! In the West, the state would help you with medicine, equipment, a wheelchair… I don’t know how it is in Russia (or wherever you live), but here in Georgia, they don’t help with anything!
You won’t believe it, but I couldn’t even get a disability sticker for my car. If I were missing a leg, I’d get it, but with COPD — no. God, I would give away my second leg too, just to be an amputee disability instead of a COPD disability.
Believe it or not, I haven’t been outside for 4—5 years, yet I cannot get the “First Group” disability status (total disability). To get it, you have to go through all the circles of hell with clinical examinations. For the Ministry of Health, no patient means no problem. So I gave up. I even receive a regular pension, because the “Second Group” pension is actually lower than the standard one — apparently, they think we can still go to work… for me, even walking to the bathroom (sorry) is a challenge. So I live with the Second Group status. And I’ve lived without doctors for about three years now — no tests, no check-ups, everything is based on my own sensations and experience.
Milana V. yurayakunin, thank you for the answer. We live in the Moscow region. A regular pulmonologist made the diagnosis. My husband had pneumonia 2 years ago, and about 8 months later, a cough started, mostly at night. I spent a long time convincing him to see a doctor. Finally, he went, and here is the diagnosis. We did a CT scan and spirometry; the disease is not advanced, more of the emphysematous type, but of course, both he and I know it will progress.
He quit smoking. He struggles with phlegm at night. He was prescribed only Spiriva® Respimat® and breathing exercises. None of the doctors say anything about disability. So if it’s not too difficult for you, please share your experience. The experience of people who have gone through the stages of the disease often provides more knowledge than the soulless words of doctors.
yurayakunin (Author) Milana, Spiriva® Respimat® is a good remedy. I used it, but there’s a problem with it in Tbilisi. It was sent to me from abroad; it was a hassle, so I gave it up. Interestingly, I didn’t notice any worsening at all. Now I use Seretide aerosol. Breathing exercises are good. There are various courses available online. If you have any questions, ask, and I will answer.
kot. hp (Natalia) yurayakunin, three years ago I was diagnosed with COPD or fibrosing alveolitis. I live in a fog, constantly sick. I looked online for groups of people with the same condition but found nothing. I’d like to talk; maybe someone can suggest how to live longer with such a disease.
yurayakunin (Author) Natalia, good day. Nothing can be done to cure this disease; you can only maintain a more or less comfortable state. Medications will be prescribed, and you will choose what suits you best, but strength of will — that depends only on you, and sometimes it is needed more than medicine. I have the bronchitic type, but the differences are in the nuances. Write about what bothers you — we’ll think about it together.
Milana V. Natalia, hello! I ordered the PARI O-PEP exerciser from a store; they deliver, and it costs about 2500 rubles. Natalia, I read about this the other day — think about a harmonica; the principle is the same. I just searched for the exerciser online, and several offers came up. My husband says it helps him; he practices twice a day for 10 minutes. He got the pneumococcal vaccine, but a doctor friend advises against the flu shot — you don’t know who to listen to, though the pulmonologist isn’t against it. The doctor says people live for 30 years with this disease; clean air is very important.
kot. hp yurayakunin, at the beginning of the illness, I had strength of will; I sought treatment and did exercises. But after the last examination, it turned out the disease is progressing. CT scans showed “honeycomb lung” — it’s all full of holes. That’s when I lost heart. All these medicines are useless. I catch every virus; it immediately turns into bronchitis, and the phlegm won’t clear. Chest pains start immediately upon inhaling. Do you take hormones or not? I’ll have to start taking them soon. I’m very afraid.
kot. hp Milana, that’s exactly what I wanted to know — is there any point in buying it? Does his phlegm clear out after using this exerciser?
Milana V. Natalia, yes, it does. Find Pulmonologist Meshcheryakova on YouTube; she’s been involved in COPD rehabilitation for 10 years. When I went to see her instead of my husband, she explained everything very clearly and showed many techniques to ease his condition — exercises to strengthen the diaphragm muscles. I highly recommend looking her up.
yurayakunin (Author) Natalia, of course I take them!!! You are preparing to die, yet you haven’t even taken hormones. I’ve been sick for 21 years and have gone through different periods. Twelve years ago, there was a time when I had to call an ambulance almost every day because around four in the morning, suffocation attacks would start. It felt like the paramedics were taking me out of a noose, and this went on for nearly a year. My wife should be awarded a “Heroine Wife” medal, but unfortunately, no such medal exists. I will write about how I got rid of that unbearable state. My dear, those who want to — find a way; those who don’t — find an excuse. Fight, but most importantly, your loved ones must help you in this struggle; you cannot conquer this road alone! And why are you afraid of hormone-containing drugs? They are the foundation of treatment — or rather, of maintaining a positive state. You can’t get anywhere without hormones. It is better to gain a little weight than to die quickly.
yurayakunin (Author) Milana, these exercises are good in themselves — a great way to maintain muscle tone — but unfortunately, exercises are useless specifically in fighting COPD.
Milana V. yurayakunin, Yuri, thank you, but surely there must be some way to support oneself.
yurayakunin (Author) Milana, of course! My wife and I have been doing this for 21 years! 21!!!!!
Severina Natalia, go get a bioresonance diagnosis; you’ll surely be surprised — someone is living in your lungs, meaning parasites.
Milana V. Natalia, someone is advising you to get some kind of bioresonance diagnosis — don’t throw your money away. I only believe in official medicine, perhaps because my mother-in-law was a chief physician at a clinic for 20 years and taught us to trust doctors and herbal treatments, but without fanaticism. Medicine does not stand still; this disease is now the 3rd most significant cause of death, and many pharmaceutical companies worldwide are working on new and more effective drugs. The author of this block has lived with this disease for 20 years and has no intention of giving up. I believe that an exchange of opinions on treatment between patients can offer a lot for maintaining health and extending life. Thank you, yurayakunin, for sharing your advice with all of us.
yurayakunin (Author) Milana, thank you. This disease is characterized by the fact that at some point, you realize all connections with the outside world are severed and you are one-on-one with the illness (read my miniature — “The Talking Head”). That is where the internet comes in handy; it helps you still feel alive. Strength of will, experience, and the desire to live — that’s already a lot. Today I live with minimal mobility but maximum comfort. You won’t believe it, but for two years, I haven’t had a single doctor at my house except for the ambulance… and a dentist :)
Milana V. yurayakunin, why wouldn’t I believe you? Usually, we visit doctors often only at the beginning of the illness, and then, having learned to listen to our bodies, we start seeking them out less frequently. No matter how good the relationship with a physician is, communicating with them is always uncomfortable: for patients, because we might ask the same thing several times and be frustrated that we didn’t get the answer we expected; and for doctors — I know from my mother-in-law, she was of the old school and upbringing — they aren’t completely indifferent and feel guilty that they cannot help the patient. In the past, very informative brochures were published about diseases; now we have the internet to help us. My husband hasn’t seen his pulmonologist for 4 months and doesn’t plan on going anytime soon, as he is slowly learning to live with his illness.
Milana V. yurayakunin, “The Talking Head” is too minor for me; I like the one about khinkali more — which I love — and the Vake district in Tbilisi. I was in Tbilisi last in 1989; our friends who live there tell us it’s completely different now.
yurayakunin (Author) Milana, good luck!
kot. hp yurayakunin, well, what kind of life is that — being tied to a hose? A friend of mine has been living like that for two years. She only dreams of falling asleep in the evening and not waking up.
yurayakunin (Author) Natalia, does your friend not have a balcony?
kot. hp yurayakunin, your sarcasm is out of place here. Why did you create these notes — to laugh at people? In what way is your “moral support” expressed? Not everyone has such strength of will as you, and not everyone has support like your wife. Many people survive however they can, and everyone’s circumstances are different; some don’t even have the opportunity to buy this oxygen machine.
yurayakunin (Author) Natalia, dear Natalia, not everyone writes poetry like Byron or plays the violin like Paganini. So what — should we burn Pushkin and tear the strings of the violin? Sarcasm is appropriate everywhere, as this is life, and everyone lives it as best they can and as the situation allows. So, if not everyone has the same strength of will as I do, should I be crucified for it? And as for my wife — she is my second wife. I suffered with my first one for 23 years, apparently so that I could receive my second wife as a reward and live with her for another 23 years. “Some don’t even have the opportunity to buy this oxygen machine.” I didn’t have the opportunity to buy an oxygen concentrator either — it was GIFTED to me. The first time it was used, and the second time it was brand new. And what’s important is that I didn’t even ask for them to be gifted!
kot. hp yurayakunin, I have nothing against you; on the contrary, I thought: there are people strong in spirit, but I, for example, am not like that, and it’s very hard for me to think that I only have 2 years of life left. And your answer about the balcony… Someone might laugh, but someone else might just take a step [off of it].
yurayakunin (Author) Natalia, how do you know about two years of life? Doctors guaranteed my wife that I had 3—4 years. 21 years have passed since then. Yes, today my condition, I think, looks like it might last a year, but I will fight. By the way, a month ago I released three of my books. I have no time to die; I’m thinking of writing another one.
A.F. Natalia, where did you see strength of will? The man sits at home with an oxygen hose for comfort, apparently, but at the same time reports that he is able to walk 50 steps. I also walk 50 steps, but I understand that you need to get out every day to the bench by the entrance, rather than staging a “Lament of Yaroslavna” [endless crying]. I don’t believe that you can’t drink a cup of coffee in that condition without oxygen… It’s just comfortable for him, he’s just used to it, that’s all. We’ve been there, we know.
Milana V. A., he doesn’t know about Yandex Zen, I’m the one who reads it.
A.F. Milana, well that’s good, otherwise he’ll read all this nonsense and sit at home without leaving, pretending to be miserable. With this disease, you quickly get used to such a lifestyle and come up with excuses for yourself not to bother with walks. It’s just hard to break the habit later. It’s an excuse. Winter, nothing more. The author of these notes is a vivid confirmation of what I wrote.
Vitaliy N. Milana V., I’ve been sick for 6 years, an extremely severe degree of COPD turning into emphysema. It is mandatory to use an inhaler, preferably one with two components. Berodual via a nebulizer. Quit smoking and drinking, definitely. Get vaccinated against pneumonia and the flu. Protect yourself from colds.
Flura T. 10 years with COPD. I’ve tried many things, and there is nothing better than Strelnikova’s breathing exercises.
yurayakunin (Author) Flura, everyone selects what works best for them. The main thing is that it helps!
yurayakunin (Author) Flura, get checked and make sure that you definitely have COPD.
A.F. yurayakunin, you should cast aside laziness and do your exercises.
Dmitry Grafov I am very ill. I think your information will help someone; maybe one day I will also write about my bitter experience.
Ayumi Hello, I have asthma and the emphysematous type of COPD. I’m 39, and I don’t smoke. I was diagnosed with COPD at 35. My disease is caused by Alpha-1 antitrypsin deficiency.
yurayakunin (Author) Ayumi, Alpha-1 antitrypsin deficiency is a hereditary disease characterized by low levels of the alpha-1 antitrypsin (A1AT) protein in the blood. Mostly, A1AT deficiency manifests as COPD, emphysema, as well as damage to the liver and blood vessels. Try to create comfortable living conditions for yourself — that is all we can do today to help ourselves. Breathe oxygen (oxygen concentrator) when you feel a lack of it — do not strain the heart. In COPD, if you don’t take care of it, the heart is the first to fail.
A.F. Ayumi, don’t listen to nonsense. A concentrator is needed not for comfort, but for use during exacerbations, if necessary. If you sit at home without going out, your heart will eventually be good for nothing. You shouldn’t be lazy; you should try to walk more. For some it’s 50 meters, for others it’s all 100.
Vladimir The information is complete, nothing to add. Thank you.
A.F. I have read all your notes. I suffer from stage 3—4 COPD myself. Your doctors are strange. With COPD, you need to get an antibiotic injection and an IV drip once every six months. I can’t imagine what I would do without this procedure. I would probably always walk around connected to an oxygen concentrator. And every year in February, I would be visiting the ICU.
Milana V. A., is it really necessary to take antibiotics? My husband has stage 1—2 and no antibiotics are prescribed to him.
A.F. Milana, I didn’t mean stage 1—2; when exacerbations occur, such a need will arise.
Milana V. A., I still don’t understand how these exacerbations manifest? There is a lot of panic due to our ignorance; please share.
A.F. Milana, don’t panic with stage 1—2. I only went to the doctors 6 years ago when I already had stage 3—4. There is nothing terrifying about your situation. I was still running when I was in your state. I think if you were to diagnose long-term smokers and those who have had pneumonia multiple times, everyone would be at stage 1, and half of them at stage 2. The author of these notes is just fear-mongering; he’s simply too lazy to crawl out of his apartment — he’s gotten used to it and convinced himself of things that aren’t there.
A.F. Milana, buy a pulse oximeter. Keep an eye on the blood oxygen level and pulse. It will make it clear when, what, and why things are happening.
yurayakunin (Author) I recently bought my fourth one. They didn’t break; I either submerged one in the bathtub, dropped another, or just lost one…
Get Examined at a Clinic
Doctor examining a chest X-ray. Try to have a family pulmonologist.
I want to say right away that I am not a doctor, but a patient; I will not give advice on specific medication, but I will tell you what I went through and how I was treated — then you can think for yourself and, most importantly, react in time.
I want to warn you about one thing: do not trust a doctor’s “sensations.” There are many doctors, and their sensations are likely to be different. Trust the results of spirometry, the determination of blood oxygen levels with a pulse oximeter, X-rays, and lung tomography. My advice is not to wait until you turn into the kind of patient whose shortness of breath is already making itself felt before running for an examination.
Run not just to a pulmonologist with a phonendoscope, but to an equipped clinic where your breathing will be checked using computer programs that exclude both your own sensations and the subjective diagnosis of a doctor. If your local clinic does not have the necessary equipment (though I think it exists everywhere now), do not be lazy and get examined at another clinic at least once a year or undergo a thorough examination — it is worth it. First of all, you will have all the results of your examinations saved, and an objective picture of the changes in your lungs over time will be visible; from these, one can roughly, but still, determine the effectiveness of the prescribed treatment.
I would not advise you to get X-rays for two reasons: first, one must be able to “read” them, but not a single pulmonologist will tell you that they cannot read them. Some doctors could almost determine my blood type from an X-ray. Most importantly, today there are much more effective methods of lung examination than X-rays that can provide a computer-generated conclusion.
And one more very important observation: smoking, of course, is harmful in any case, but COPD does not only appear from smoking, like a pregnancy from a sperm cell — it increasingly occurs due to environmental factors, which, of course, the state will never admit to you. Apparently, all Russians think that the cars stuck in traffic jams are exhaust pipes belching out oxygen? Look first at the quality of gasoline at the gas stations and how many cars are equipped with the modern exhaust systems that are mandatory in the West. People in the “soviet-style” system apparently think that factory chimneys are all equipped with harmful substance traps, and that the smoldering piles of garbage located right next to city blocks are smoking with Indian incense?
Think about it: if all the trouble comes from tobacco, why have people started smoking less, while COPD has started appearing more frequently? As long as you keep smoking, as long as factory chimneys and mountains of garbage continue to smolder near housing, as long as there is leaded gasoline and no exhaust catalysts — you will suffer from COPD, and your children might start suffering from it from childhood. So, you will have to walk around in respirators if the state, unlike the West, couldn’t care less about the environment in the country.
I think I have written enough so that those who read my article and possess a sufficient amount of gray matter in their heads will go and check their lungs tomorrow, because at early stages the process can be somewhat arrested, but at late stages — alas.
Suffocation
Since childhood, my health had been excellent — so much so that I suffered through pneumonia several times “on my feet,” and neither I nor my parents even noticed. At home, illnesses were treated according to the proverb — “It will heal before the wedding”. Not everything healed, and I periodically suffered from bronchitis, which I also endured without staying in bed, as it didn’t bother me with anything except a cough and phlegm; no one even suspected future problems. My grandmother suffered from asthma, but I never saw any asthma medication in the house. My dear parents, do not make irreparable mistakes: “it will heal before the wedding” only applies to what you actually treat in a child yourselves.

Note: This image powerfully visualizes the sensation of air hunger described in the text.
So, now you know that my lungs were my weak point since childhood. However, because I was a swimmer and my “breathing capacity” was well-developed, I didn’t experience any particular problems with my breath or lungs — except perhaps in the 90s, when for ten years in Georgia there was no light, no gas, and consequently no heating. During that time, bronchitis and coughing became frequent guests, but when the heating was sorted out and the need to sleep in clothes vanished, everything seemed to pass — but, apparently, only “seemed”.
One fine December evening in 1998, out of nowhere, I suddenly felt such an attack of suffocation that I simply crawled out onto the balcony, but the attack would not pass. Nothing like this had ever happened to me before. I sat in a chair and breathed like a fish thrown onto the shore; there wasn’t enough air. I felt so bad that the thought “this is it — the end” crept into my mind.
My wife and mother-in-law didn’t know how to help and called the ambulance three times. The poor doctors had to climb to the eighth floor on foot because there was no electricity for the elevator. Since this condition was a first for me, we couldn’t tell the doctors anything specific. The doctors assumed I was having an asthma attack, gave me Astmopent to breathe, injected something, said it would pass in ten to fifteen minutes, and left.
The second ambulance didn’t help either; they simply let me breathe some oxygen. On the third visit, after four hours of agony, I asked them to inject a sedative because I could no longer endure the suffering. I woke up the next day feeling “fresh as a daisy,” with no problems at all except for abdominal pain — my stomach muscles were sore from the long, intense breathing.
Of course, Lika insisted I see doctors immediately, from “celebrities” to acquaintances. I hadn’t yet heard of the acronym COPD, and the diagnoses were striking in their variety: from asthma and allergies to a deviated septum, with congenital genetic diseases and psychiatric disorders in between. It would have been fine if these were just diagnoses, but all these doctors promised to “put me back on my feet” in two or three weeks and treated me with aggressive methods for an aggressive fee. A month later, they would declare that I must have “something else” and advise me to see another doctor, immediately providing a name and phone number.
The last person who tried to cure me “on the fly” was a maxillofacial surgeon who suggested an operation to correct my nasal septum. At that point, my patience snapped, and I stated that if the operation didn’t help, I would perform “surgery” on his face with my fists; after that, they decided not to do the operation.
Meanwhile, my health worsened. The attacks became more frequent — perhaps not as acute as the first one, or maybe I was just getting used to them — but more frequent. My general condition deteriorated to the point where I couldn’t hold my son in my arms; I could only carry him by sitting him on my neck. Externally, my breathing became sharp and “chest-heavy”.
To understand the level of competence of “Soviet-style” pulmonologists, I will cite the diagnoses given to Soviet luminaries when no one knew anything about COPD. When the body of the proletarian writer Maxim Gorky was autopsied after his death, witnesses stated: “the condition of the lungs was terrible. Both lungs had almost entirely ‘calcified,’ and the bronchi looked just as horrific. It was unclear how he breathed at all”. The version that Gorky was poisoned with candy was not confirmed; the cause of death was a long-standing illness. Today, it is believed the writer was treated incorrectly: they treated him for asthma, but they should have treated him for COPD.
The diagnosis for the leader of the USSR, Konstantin Chernenko — “pulmonary emphysema” — was also incorrect. The famous director Oleg Efremov was diagnosed with “pneumoneurosis” and “pulmonary heart”. He died of suffocation. I believe that since the Soviet era, the competence of doctors has not only failed to increase — it has likely degraded.
Panic Attack

When I write about COPD, I relive everything all over again: the time when I could break an arcade machine in the city park with a single blow, and the time when I thought that stepping off the balcony of the eighth floor (I live on the 19th floor now, but back then it was the eighth) would bring relief to everyone.
To understand what daily suffocation attacks in the early morning hours are like — the calls to the paramedics and the agonizing wait for their arrival — one must experience these attacks firsthand. I wouldn’t wish them on my worst enemy.
During suffocation, you experience a subcortical, uncontrollable, wild terror. It is likely the kind of terror experienced by those condemned to hanging from the moment they feel the noose on their neck until they lose consciousness. But unlike them, you do not lose consciousness; you simply lose control of it because you are in the grip of a panic attack.
Until the ambulance arrives, until they inject dexamethasone into your veins (which are already in worse shape than a drug addict’s), and until you are connected to oxygen — your brain is in charge of your survival. This survival consists of shutting down the body’s secondary functions to conserve oxygen. Just imagine what functions the brain shuts down to save oxygen for the heart and the head.
Everyone experiences anxiety or fear from time to time, but a panic attack is of a much higher intensity. It is accompanied by trembling, a racing heart, sweating, and numbness. There is a feeling that something horrific is about to happen. During a PA (panic attack), a person is unable to control their fear, internal sensations, or certain actions. The brain seems to fall out of reality, held captive by these experiences.
On average, a panic attack lasts half an hour. It poses no physical danger, but the individual struggles to perceive reality because they are governed by a deep fear — including the fear of death. Imagine this happening almost every day, and you will understand my state and the state of those around me.
Бесплатный фрагмент закончился.
Купите книгу, чтобы продолжить чтение.
